If you have ever sought breast reduction surgery on the NHS, you may have come up against a wall of criteria that feels arbitrary — and, for many women, deeply unfair. To qualify, you typically need a BMI below 26–28 (the threshold varies by region), your surgeon must plan to remove more than 500 grams of tissue per breast, and you must be a non-smoker. Tick all three boxes and you might be considered. Miss even one and you are turned away.
These criteria are measurable. They are auditable. And they almost entirely miss why breast reduction surgery matters.
What the Criteria Get Right — and Wrong
The physical benefits of breast reduction are real and well-documented. Women with very large breasts frequently suffer chronic back and neck pain, shoulder indentation from bra straps, skin rashes and infections beneath the breast fold, and restricted breathing during exercise. These are legitimate medical concerns, and the NHS criteria attempt to capture them — the 500-gram threshold is a proxy for "large enough to cause functional problems."
But the criteria draw a sharp line between the body and the mind, and in doing so, they ignore a substantial body of evidence.
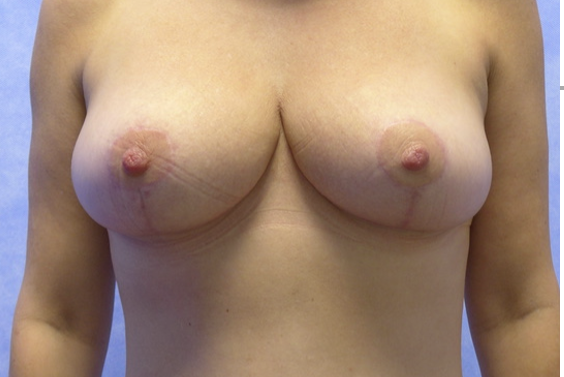
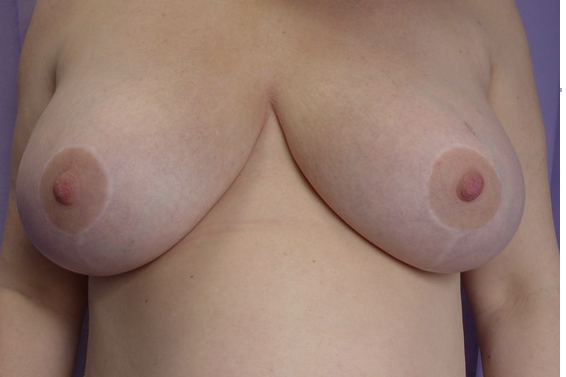
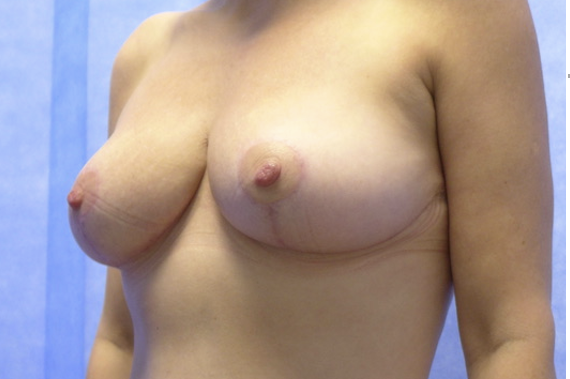
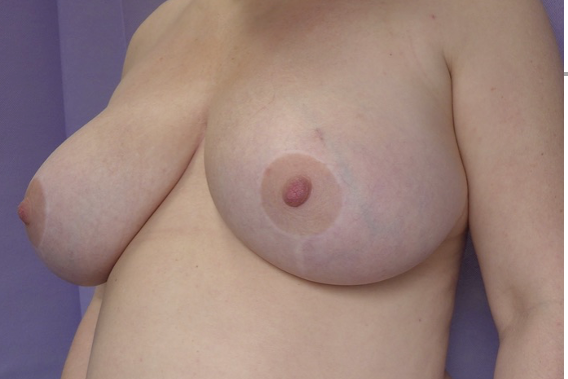
This patient sought a redo breast reduction and abdominoplasty. She was advised to reach her happy weight before surgery and lost 20kg. She then had successful combined surgery. Shown at 3 months post-operatively, when scars are at their most noticeable. Drag the slider to compare before and after. Published with written patient consent.
The Psychological Burden Nobody Is Measuring
Published research in the Journal of Plastic, Reconstructive & Aesthetic Surgery makes the case plainly: "Cosmetic surgery is psychotherapeutic." The degree of distress a patient experiences should matter at least as much as the volume of tissue removed — and for breast reduction, the psychological impact is often profound.
Consider what a young woman with disproportionately large breasts may actually be living with. She may have stopped playing sport. She may wear loose, unfashionable clothing to disguise her figure. She may hunch her shoulders forward, avoid mirrors, refuse to undress with the lights on. She may have withdrawn from friends, given up hobbies, or changed her entire personality — not because she is anxious by nature, but because her body draws unwanted attention she never asked for. One patient, describing her experience at the age of eleven, recalled being made to feel "strange and uncomfortable" by an adult male's attention to her developing breasts. These experiences leave marks that BMI cannot capture.
Older women seeking breast reduction face a different but equally real burden: years of carrying weight that causes pain, limits activity, and erodes confidence. For both groups, the improvement in quality of life after surgery is often greatest not because the back pain is gone — but because the psychological distress is resolved.
The appropriate measure for surgical intervention is "not the grossness of the abnormality, but the degree of emotional distress that the abnormality of appearance produces."
— Harris, cited in Blackburn & Blackburn (2008)
A Postcode Lottery Built on an Incomplete Picture
The NHS's approach creates two particular injustices.
First, the BMI threshold is blunt. A woman with a BMI of 29 suffering severe psychological distress and physical symptoms may be turned away, while a woman with a BMI of 25 and less severe symptoms qualifies. Geography makes this worse: the threshold varies from area to area, meaning where you live — not how much you are suffering — partly determines your access to care.
Second, the 500-gram rule means that women with smaller frames, for whom even moderately large breasts create significant physical and emotional burden, may not meet the surgical threshold. The ratio of breast to body matters; the absolute weight alone does not tell the whole story.
What the Private Sector Does Differently: "Happy Weight"
One concept used by experienced surgeons in private practice illustrates just how crude the NHS BMI threshold really is. Rather than asking what a patient weighs today, a thoughtful surgeon asks: what is this person's happy weight — the weight they are realistically likely to maintain over the next ten years?
This matters because breast reduction surgery produces its best long-term results when a patient's weight is stable. Someone who is currently slightly above a BMI threshold but has been broadly the same weight for years, eats well, and exercises regularly may actually be a better surgical candidate than someone who sits just inside the threshold but whose weight fluctuates significantly. The snapshot BMI on the day of assessment tells you very little about what a patient's body will look like in five years' time, or whether the surgical result will be durable.
Happy weight is not a licence to ignore health entirely — quite the opposite. Being in good general health, and being a non-smoker, are genuinely important for safe surgery and good outcomes. Smoking impairs wound healing, increases the risk of infection, and significantly raises the chance of complications following any procedure involving large skin flaps — as breast reduction does. These are not arbitrary bureaucratic hurdles; they reflect real clinical risk. A patient who smokes is at substantially higher risk of wound breakdown, poor scarring, and nipple complications. Surgeons in both the NHS and private sector are right to take this seriously.
The distinction, however, is between health as a genuine clinical consideration and BMI as a blunt rationing tool. A woman who is fit, active, non-smoking, and stable at a BMI of 30 may be a far safer and more appropriate candidate for surgery than the BMI threshold alone would suggest. What matters is the whole picture — her health, her stability, and yes, her suffering.
What Should Change
Rationing in the NHS is an unavoidable reality, and nobody is suggesting that every request for breast reduction should be funded without question. But the criteria used should reflect the full range of harm the condition causes. A structured assessment of psychological impact — asking about avoidance behaviour, self-image, the effect on relationships, sport, clothing, and daily life — would give a far more accurate picture of need than a set of measurements alone. And weight thresholds should account for a patient's realistic long-term weight, not just the number on the day.
Breast reduction surgery has one of the highest patient satisfaction rates of any elective procedure. Women who have it consistently report improvements not just in physical symptoms, but in confidence, mental health, and overall quality of life. To ration access based on a scale and a set of scales, while ignoring the person holding them, is to misunderstand what the operation actually does.
