A great many women come to see me not because they dislike how they look, but because they cannot do things they used to do. They cannot run without lower back pain. They cannot lift without their abdomen bulging outwards in a way that feels wrong and sometimes hurts. Their pelvic floor is weak, and some cannot jump on a trampoline with their children without worrying about leaking. A few describe an uncomfortable sensation of bowel sitting in a gap between their abdominal muscles, particularly during exertion. Some have been to physiotherapy for years without meaningful improvement.
Nearly all of them have been pregnant. And most of them have been told, at various points, to do more Pilates.
For a significant number of these women, Pilates is not the answer. No amount of it will be. The reason is diastasis recti: the separation of the rectus abdominis muscles along the midline that occurs during pregnancy as the uterus expands. In mild cases, the gap closes naturally in the months after delivery, or with targeted physiotherapy. In more severe cases, it does not close, and the connective tissue joining the two muscle bellies stretches and thins to the point where it can no longer perform its mechanical function. When that happens, the only reliable solution is surgical repair.
Where Physio Ends and Surgery Begins
The question of when conservative treatment becomes futile is one I have thought about carefully, and it is where my collaboration with Dr Sarah Rollins has been particularly valuable. Sarah is a Consultant in Sport and Exercise Medicine with a specialist interest in musculoskeletal ultrasound. She developed the Ministry of Defence ultrasound protocol for diagnosing diastasis recti abdominis, co-wrote the Defence Women's Health Rehabilitation Best Practice Guidelines, and served as MOD Lead Doctor for the Women's Health Rehabilitation Working Group. Before her recent move to Edinburgh I worked with Sarah for five years, with excellent results for our shared patients. She can now be found consulting at Pure Sports Medicine in Edinburgh, where she works closely with a local plastic surgeon for suitable cases.
Much of her clinical experience has been with post-pregnancy military personnel. These are not women who gave up on exercise. They returned to training as soon as they were permitted to and worked at it consistently. Many of them still could not recover the core function they needed. What Sarah has observed in her practice, and what is borne out by the clinical evidence, is that in women of average build, a diastasis wider than approximately 4 to 5 centimetres is unlikely to respond to conservative treatment. The gap is simply too large. The linea alba has been stretched beyond its elastic limit. Asking a muscle to generate tension through a structure that can no longer transmit that tension efficiently is like trying to pull a rope with a frayed section in the middle: the effort goes in, but the force does not transfer. Core exercises may strengthen the individual muscles but cannot restore the integrity of the midline.
Beyond a certain width, surgery is not an optional extra. It is the only thing that will actually fix the problem.
What These Women Are Actually Living With
The functional consequences of a large untreated diastasis are often underappreciated, including by clinicians. Lower back pain is the most common complaint. The deep abdominal muscles form part of a pressure-generating system that stabilises the lumbar spine during movement. When that system is disrupted, the back has to compensate, and over time it starts to protest. Women often present having already seen orthopaedic surgeons, pain specialists, and osteopaths, none of whom identified the diastasis as the underlying cause.
Pelvic floor weakness is closely related. The pelvic floor and the deep abdominal muscles work together as part of the same pressure-regulating mechanism. Weakness or poor coordination in one tends to affect the other. This is why some women with significant diastasis experience symptoms that look primarily like pelvic floor dysfunction: urinary leakage, difficulty with impact exercise, discomfort during intercourse. The trampoline is a useful illustration: the inability to jump with their children is not a minor inconvenience, it is a daily reminder of what the condition has taken from them.
The visible consequences carry their own burden. Abdominal doming, the outward bulging of the midline that becomes apparent during movement or exertion, is something many of these women manage constantly. They select clothes specifically to disguise it. When sitting in company, they position a handbag or a cushion across their lap. Several patients have described being asked by strangers whether they are expecting another child. That question, asked innocently, lands with considerable force for a woman who has spent years trying to conceal the physical legacy of her pregnancies. The cumulative weight of managing a visible deformity, socially and psychologically, is not trivial and deserves to be taken seriously.
A smaller number of patients describe something that sounds unusual until you think about the anatomy: a sensation of abdominal contents, sometimes specifically the bowel, moving into the gap between the muscles during exertion or at rest. This is not a hernia in the traditional sense, but it is not comfortable, and it does not resolve without closing the gap.
The Operation and What It Achieves
The surgical repair involves bringing the two muscle bellies back together in the midline and securing them there with permanent sutures. This is the plication component of an abdominoplasty. It restores the mechanical integrity of the abdominal wall: the muscles can now function as a unit, core stability improves, and the lower back is better supported. For women who had significant functional symptoms beforehand, the relief is often striking.
The abdominoplasty component addresses the loose skin and stretched abdominal wall that pregnancy leaves behind. The skin below the umbilicus, which is often the most affected, is excised. The umbilicus is repositioned. The result is a flatter, firmer abdominal contour. For many patients, this improvement in silhouette matters to them, but I want to be clear: it is secondary to the functional repair. The operation is justified on functional grounds. The aesthetic benefit is real, but it is not why these women need surgery.
Abdominoplasty is also psychotherapeutic. Harris, writing on the relationship between appearance and surgical intervention, put it clearly: the application of cosmetic surgery should be judged not on the grossness of the abnormality, but on the degree of emotional distress that the abnormality of appearance produces. Prospective evidence supports this: abdominoplasty is associated with significant improvements in quality of life, body image, psychological distress, and self-esteem. For women who have spent years managing both debilitating physical symptoms and the social burden of a changed body, the relief tends to be substantial. Patients describe putting on clothes they had not worn since before their pregnancies, getting back into the pool with their children, and, quite simply, feeling like themselves again.
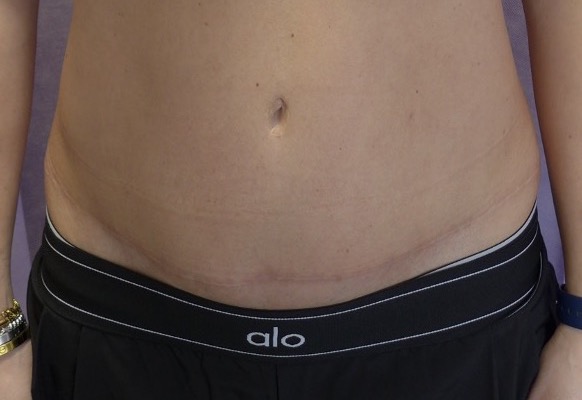
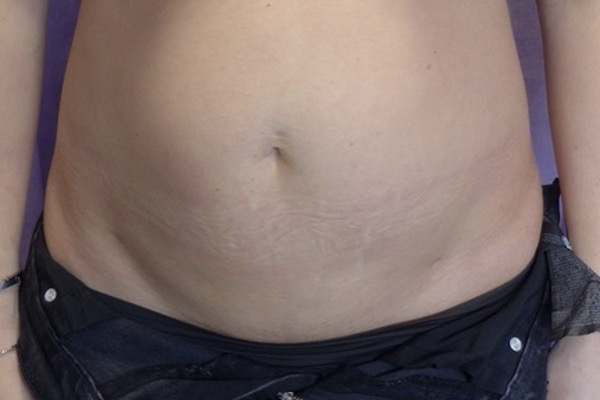
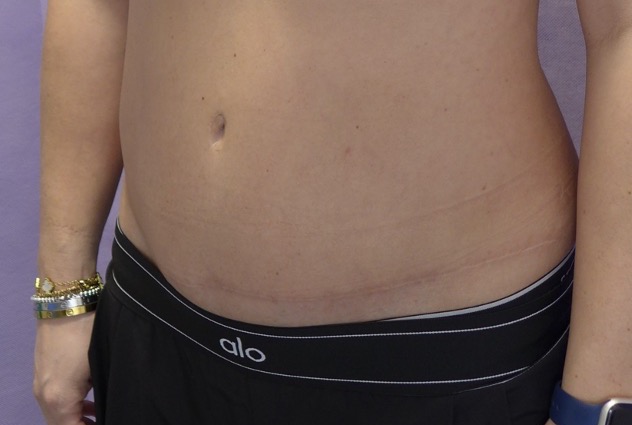
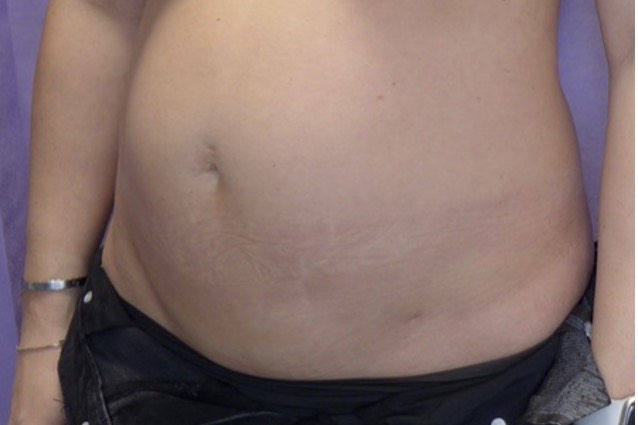
Abdominoplasty with rectus plication. Shown at 20 months post-operatively. Drag the slider to compare before and after. Published with written patient consent.
Who Is a Suitable Candidate
The ideal candidate for functional abdominoplasty has completed her family, is in good general health, is a non-smoker, and has given conservative treatment a genuine chance. That last point matters: surgery is not a shortcut past physiotherapy, and patients who have not yet worked with a specialist physiotherapist should do so first. For many women, that will be sufficient. For those with a large diastasis who have already tried, it confirms that they have reached the limit of what conservative treatment can offer.
Weight stability is also important. Significant weight gain after surgery can re-stretch the abdominal wall and compromise the repair. I use the same concept here as I do in breast surgery: I want to know a patient's happy weight, the weight she is realistically going to maintain, not the weight she happens to be on the day of the consultation.
Smoking is an absolute contraindication. Abdominoplasty involves a large skin flap, and healing in smokers is substantially impaired. The risk of wound breakdown, infection, and fat necrosis is too high to accept.
A Word on Prehabilitation
Working with Dr Sarah Rollins has reinforced something I believe strongly: the best surgical results come from patients who are as strong as possible before the operation. Prehabilitation, targeted exercise and conditioning in the weeks before surgery, improves recovery times, reduces complications, and means the rehabilitated abdominal wall has better muscle to work with once the repair is done. Patients who arrive in good physical shape, even if their core function is compromised, tend to do better than those who have been largely inactive.
For patients referred through Dr Rollins, we work as a team. She assesses and prepares them, I operate, and she supports their recovery afterwards. That continuity, and the depth of her expertise in this specific area, makes a real difference to outcomes.
The Conversation I Have Most Often
The most common thing I hear in clinic is some version of: "I've been told this is just what happens after having children and I need to live with it." Sometimes that is true. Often, for women with a small diastasis and mild symptoms, it is. But for women with a wide separation, significant functional symptoms, and a long history of unsuccessful conservative treatment, it is not true. There is a surgical solution, it works, and they deserve to know about it.
Abdominoplasty has a reputation as a cosmetic operation for women who want a flat stomach. For a proportion of my patients, that reputation is a barrier: they do not think of themselves as the kind of person who has cosmetic surgery, and they are not sure a surgeon will take their functional symptoms seriously. I want to be clear that functional indications are entirely legitimate and that they are, for many patients, the primary reason for operating. The improved silhouette is welcome. Getting your body back is the point.
